Connect With Us
Blog

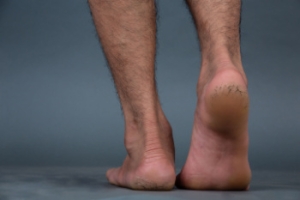
Cracked Heels and Their Causes
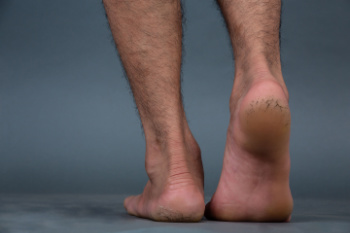
Cracked heels occur when the skin on the heels becomes dry, thickened, and splits. These cracks can cause discomfort and lead to infections if left untreated. The primary causes of cracked heels include dry skin, which reduces skin elasticity, and excessive pressure from standing or walking for long periods. Poor footwear choices, such as shoes that do not provide adequate support, can worsen the condition. Certain medical conditions like diabetes and eczema can also contribute to cracked heels, as they affect the skin’s ability to retain moisture. Obesity adds extra pressure on the feet, increasing the risk of cracks or fissures. Additionally, hydration is essential for maintaining skin health, and drinking sufficient water helps prevent the skin from drying out and cracking. Cracked heels can be painful and make it difficult to complete daily activities. If you have developed this condition, it is suggested that you consult a podiatrist who can successfully treat this ailment, which may include prescribed medication.
If the skin on your feet starts to crack, you may want to see a podiatrist to find treatment. If you have any concerns, contact one of our podiatrists from Lexington Foot and Ankle Center, PSC. Our doctors can provide the care you need to keep you pain-free and on your feet.
Cracked Heels
It is important to moisturize your cracked heels in order to prevent pain, bleeding, and infection. The reason cracked heels form is because the skin on the foot is too dry to support the immense pressure placed on them. When the foot expands, the dry skin on the foot begins to split.
Ways to Help Heal Them
- Invest in a good foot cream
- Try Using Petroleum Jelly
- Ease up on Soaps
- Drink Plenty of Water
Ways to Prevent Cracked Heels
- Moisturize After Showering
- Skip a Shower
- Keep Shower Water Lukewarm
- Don’t Scrub Your Feet
If you are unsure how to proceed in treating cracked heels, seek guidance from a podiatrist. Your doctor will help you with any questions or information you may need.
If you have any questions, please feel free to contact our offices located in Harrodsburg, Frankfort, Georgetown, and Lexington, KY . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Solutions for Cracked Heels
Cracked heels may make you want to think twice about showing off your feet in warmer weather. However, cracked heels may be harmful to more than just the appearance of your feet. If deep fissures and cracks develop in your heels, they may make walking and standing painful for you. Additionally, these openings make way for germs to enter through your skin and cause infection.
There are several different causes of cracked heels. One of the most common reasons for this ailment is dry skin. This problem may make your keeps feel rough tight and itchy. Dry skin may be caused by cold air, extremely hot water, harsh soaps, and aging. Skin disorders such as eczema and psoriasis may eventually lead to dry skin. In some cases, complications may arise from cracked heels. Some of these complications are a loss of feeling in the heel, cellulitis, or a diabetic foot ulcer.
There are ways you can try to prevent getting cracked heels. One of the best ways to do so is to avoid wearing flip flops and sandals because these shoes increase your risk of drying out your feet. You should also avoid wearing shoes with a tall skinny heel, because these shoes cause your heel to expand sideways. At night, you should slather on a thick moisturizing cream on your feet and then cover them in socks to keep your feet moisturized overnight. Drinking water to stay hydrated is also a good way to ensure that your skin doesn’t become dry.
If you suffer from a severe case of cracked feet, you should make an appointment with your podiatrist to see what treatment methods are best for you.
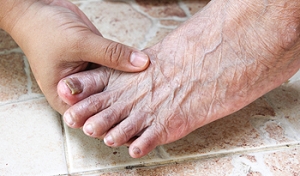
What to Do With Thick Toenails
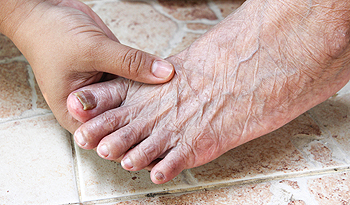
Thick toenails are a common condition where the toenails become abnormally thick, often appearing yellowish or discolored. This condition can be caused by fungal infections, aging, trauma to the toenail, or underlying health conditions like diabetes or psoriasis. The symptoms of thick toenails include visible thickening, discoloration, and sometimes crumbling or brittle edges. The toenails may also become painful, especially when pressure is applied, or when wearing tight shoes. In severe cases, the nail may lift from the nail bed or become misshapen. Treatment for thick toenails depends on the cause. If caused by a fungal infection, antifungal medications, either topical or oral, are typically used. In some cases, a podiatrist may recommend trimming or debriding the toenail, or using laser therapy to treat fungal infections. A podiatrist can diagnose the underlying cause and provide effective treatments for thick toenails. If you are experiencing this condition, it is suggested that you make an appointment with a podiatrist.
If left untreated, toenail fungus may spread to other toenails, skin, or even fingernails. If you suspect you have toenail fungus it is important to seek treatment right away. For more information about treatment, contact one of our podiatrists of Lexington Foot and Ankle Center, PSC. Our doctors can provide the care you need to keep you pain-free and on your feet.
Symptoms
- Warped or oddly shaped nails
- Yellowish nails
- Loose/separated nail
- Buildup of bits and pieces of nail fragments under the nail
- Brittle, broken, thickened nail
Treatment
If self-care strategies and over-the-counter medications does not help your fungus, your podiatrist may give you a prescription drug instead. Even if you find relief from your toenail fungus symptoms, you may experience a repeat infection in the future.
Prevention
In order to prevent getting toenail fungus in the future, you should always make sure to wash your feet with soap and water. After washing, it is important to dry your feet thoroughly especially in between the toes. When trimming your toenails, be sure to trim straight across instead of in a rounded shape. It is crucial not to cover up discolored nails with nail polish because that will prevent your nail from being able to “breathe”.
In some cases, surgical procedure may be needed to remove the toenail fungus. Consult with your podiatrist about the best treatment options for your case of toenail fungus.
If you have any questions, please feel free to contact our offices located in Harrodsburg, Frankfort, Georgetown, and Lexington, KY . We offer the newest diagnostic and treatment technologies for all your foot care needs.
How to Treat Your Toenail Fungus
While not a serious issue, toenail fungus, or onychomycosis, can be an embarrassing and uncomfortable condition to experience. Toenail fungus is often caused from public areas that harbor fungi and improper cleaning/drying of the foot. Once infected, the fungus grows deeper into the nail and can be very hard to get rid of.
There are different types of fungus that cause toenail fungus. Dermatophytes, yeasts, and molds are the most frequent forms of fungus to infect the toenail. Dermatophytes are the most common among the three. Symptoms associated with fungal nails include the discoloration of the toenail, brittleness, and in some circumstances, a smell. Pain is rarely a symptom caused by toenail fungus.
Diagnosis of fungal nails is generally a rather quick process. However podiatrists will make sure that the cause is not another condition such as lichen planus, psoriasis, onychogryphosis, or nail damage. Podiatrists will make use of fungal cultures and microscopy to verify that it is fungus.
While over-the-counter ointments are readily available, most are ineffective. This is due to the fact that the nail is very protective and that the fungus slips in between the nail plate and bed. Podiatrists can offer oral medication which currently provides the best results.
Ultimately, prevention is the best line of defense against toenail fungus. Avoid unsanitary public showers. If you do use a public shower, use shower shoes to provide your foot with protection. Once you are finished showering, make sure to thoroughly dry your feet. Fungi thrive in warm, dark, and moist places like sweaty, warm feet that are left dark in shoes all day.
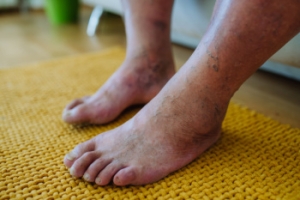
Preserving Mobility and Health With Lower Limb Salvage
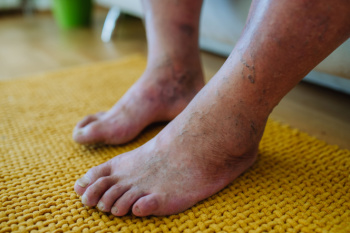
Lower limb salvage focuses on saving an at-risk leg or foot from limb loss due to severe injuries, infections, or complications from conditions like diabetes or peripheral artery disease. The goal is to restore functionality, preserve mobility, and improve quality of life while minimizing pain and complications. This task requires a multidisciplinary approach and often involves advanced techniques such as wound debridement, skin grafts, vascular procedures, and reconstructive surgery. Custom orthotics, braces, or special footwear may also be used to offload pressure and prevent further damage. Early intervention is critical, as untreated infections or poor circulation can escalate quickly. Lower limb salvage is a highly personalized process that considers each patient’s unique circumstances, focusing on long-term outcomes and independence. If you or a loved one are at risk, it is suggested that you include a podiatrist on your medical team to explore the best treatment options for preserving limb health and mobility.
Diabetic Limb Salvage
Diabetic limb salvage can be an effective way in preventing the need for limb amputation. If you have a foot ulcer and diabetes, consult with one of our podiatrists from Lexington Foot and Ankle Center, PSC. Our doctors will assess your condition and provide you with quality foot and ankle treatment.
What Is Diabetic Limb Salvage?
Diabetic limb salvage is the attempt of saving a limb, such as the foot, that has an infected ulcer, from amputation. Podiatrists also try to make sure that there is enough function in the foot after the salvage that it is still usable. Those with diabetes experience poor blood circulation, which prevents proper healing of an ulcer. If the ulcer is left uncheck, it could become infected, which could result in the need for amputation.
Diabetes is the number one cause of non-traumatic amputations in the United States. Amputation has been found to lead to higher mortality rates. This translates into higher healthcare costs, and a reduced quality of life and mobility for amputees. Podiatrists have attempted to increase the prevalence of limb salvage in an attempt to solve these issues.
Diagnosis and Treatment
Limb salvage teams have grown in recent years that utilize a number of different treatments to save the infected limb. This includes podiatrists that specialize in wound care, rehabilitation, orthotics, and surgery. Through a combination of these methods, limb salvage has been found to be an effective treatment for infected limbs, and as an alternative to amputation. Podiatrists will first evaluate the potential for limb salvage and determine if the limb can be saved or must be amputated.
If you have any questions, please feel free to contact our offices located in Harrodsburg, Frankfort, Georgetown, and Lexington, KY . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Diabetic Limb Salvage
Limb salvage is a procedure that involves saving a lower extremity from amputation. In podiatry, limb amputation often occurs as a result of diabetes. The fundamental goal of limb salvage is to restore and maintain stability and movement of the affected lower extremity.
The procedure typically involves removing the diseased tissue and a small portion of the surrounding healthy tissue, as well as the removal of any affected bone if necessary. If bone is removed it is then replaced with prostheses, or synthetic metal rods or plates, or grafts from either the patient’s body or a donor. Limb salvage is typically the preferred choice of procedure over amputation, as the procedure preserves both the patient’s appearance and allows for the greatest possible degree of function in the affected limb.
Upon diagnosis and determining that limb salvage is the appropriate treatment, the podiatrist may enlist the help of a physical and/or occupational therapist to prepare the patient for surgery by introducing various muscle-strengthening, walking, and range of motion exercises. Such exercises may be continued as rehabilitation post-procedure.
Managing Gout
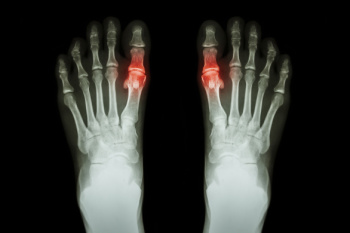
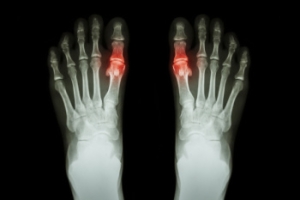
Gout is a type of arthritis caused by the buildup of uric acid crystals in the joints, often affecting the big toe. It occurs when the body produces too much uric acid or does not excrete enough through urine. Symptoms include sudden, intense pain, redness, swelling, and warmth in the affected joint, typically during the night. Gout attacks can feel excruciating, making even the lightest touch unbearable. Treatment for gout involves medications like nonsteroidal anti-inflammatory drugs called NSAIDs, colchicine, or corticosteroids to reduce pain and inflammation. Long-term management may include medications to lower uric acid levels and lifestyle changes like reducing alcohol intake and eating a purine-free diet. A podiatrist can help diagnose gout, manage flare-ups, and provide advice on footwear and exercises to reduce strain on affected joints. If you are experiencing symptoms of gout, it is suggested that you schedle an appointment with a podiatrist for effective treatment and management.
Gout is a foot condition that requires certain treatment and care. If you are seeking treatment, contact one of our podiatrists from Lexington Foot and Ankle Center, PSC. Our doctors will treat your foot and ankle needs.
What Is Gout?
Gout is a type of arthritis caused by a buildup of uric acid in the bloodstream. It often develops in the foot, especially the big toe area, although it can manifest in other parts of the body as well. Gout can make walking and standing very painful and is especially common in diabetics and the obese.
People typically get gout because of a poor diet. Genetic predisposition is also a factor. The children of parents who have had gout frequently have a chance of developing it themselves.
Gout can easily be identified by redness and inflammation of the big toe and the surrounding areas of the foot. Other symptoms include extreme fatigue, joint pain, and running high fevers. Sometimes corticosteroid drugs can be prescribed to treat gout, but the best way to combat this disease is to get more exercise and eat a better diet.
If you have any questions please feel free to contact our offices located in Harrodsburg, Frankfort, Georgetown, and Lexington, KY . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Everything You Need to Know About Gout
Gout, typically found in diabetic patients, is an unusually painful form of arthritis caused by elevated levels of uric acid in the bloodstream. The condition typically strikes the big joint on the big toe. It has also been known to strike the knees, elbows, fingers, ankles and wrists—generally anywhere that has a functioning, moving joint.
The high level of uric acid in a person’s bloodstream creates the condition known as hyperuricema—the main cause of gout. Genetic predisposition occurs in nine out of ten sufferers. The children of parents who suffer gout will have a two in ten chance of developing the condition as well.
This form of arthritis, being particularly painful, is the leftover uric acid crystallizing in the blood stream. The crystallized uric acid then travels to the space between joints where they rub, causing friction when the patient moves. Symptoms include: pain, redness, swelling, and inflammation. Additional side effects may include fatigue and fever, although reports of these effects are very rare. Some patients have reported that pain may intensify when the temperature drops, such as when you sleep.
Most cases of gout are easily diagnosed by a podiatrist’s assessment of the various symptoms. Defined tests can also be performed. A blood test to detect elevated levels of uric acid is often used as well as an x-ray to diagnose visible and chronic gout.
Treatment for gout simply means eliminating symptoms. Non-steroid anti-inflammatory drugs or NSAIDs (Colchicine and other corticosteroid drugs, etc.) will quell the redness, the swelling, and the inflammation. However, managing your diet, lifestyle changes, and using preventative drugs are all helpful toward fully combating the most severe cases.
Those that lead an inactive lifestyle are at a higher risk for gout. Any amount of exercise decreases the probability of repeat encounters with the condition. Reducing your consumption of red meat, sea food, and fructose-sweetened drinks also reduces the likelihood of chronic gout as well.
Ingesting Vitamin C, coffee, and particular dairy products can help with maintaining a healthy lifestyle. There are new drugs out on the market that inhibit the body’s production of uric acid-producing enzymes. However, reducing or eliminating your overall levels of uric acid is the best remedy to ensuring you lead a gout-free life.
Complex Foot and Ankle Injuries

Complex injuries of the foot and ankle involve multiple fractures, dislocations, or significant damage to soft tissues, such as ligaments, tendons, or nerves. These injuries are considered complex due to their intricate anatomy, weight-bearing function, and the challenge of restoring mobility, stability, and alignment. Polytrauma, where multiple injuries are affecting different areas of the body, can complicate foot and ankle injuries further, as they may be overlooked initially while treating life-threatening conditions. Such scenarios often occur in car accidents, falls, or severe sports injuries, where the foot and ankle are subject to extreme forces. Addressing complex injuries requires prompt medical attention from specialists such as podiatrists. Advanced imaging like CT or MRI scans may be necessary to fully assess the damage. Treatment typically involves surgery, targeted exercises, and long-term care to optimize recovery and restore function. If you have sustained any foot or ankle injury, it is strongly suggested that you seek care from a podiatrist.
Foot and ankle trauma is common among athletes and the elderly. If you have concerns that you may have experienced trauma to the foot and ankle, consult with one of our podiatrists from Lexington Foot and Ankle Center, PSC. Our doctors will assess your condition and provide you with quality foot and ankle treatment.
Foot and ankle trauma cover a range of injuries all over the foot; common injuries include:
- Broken bones
- Muscle strains
- Injuries to the tendons and ligaments
- Stress fractures
Symptoms
Symptoms of foot and ankle injuries vary depending on the injury, but more common ones include:
- Bruising
- Inflammation/ Swelling
- Pain
Diagnosis
To properly diagnose the exact type of injury, podiatrists will conduct a number of different tests. Some of these include sensation and visual tests, X-rays, and MRIs. Medical and family histories will also be taken into account.
Treatment
Once the injury has been diagnosed, the podiatrist can than offer the best treatment options for you. In less severe cases, rest and keeping pressure off the foot may be all that’s necessary. Orthotics, such as a specially made shoes, or immobilization devices, like splints or casts, may be deemed necessary. Finally, if the injury is severe enough, surgery may be necessary.
If you have any questions, please feel free to contact our offices located in Harrodsburg, Frankfort, Georgetown, and Lexington, KY . We offer the newest diagnostic and treatment technologies for all your foot care needs.